Greek doctors and hospital managers are drowning in paperwork, fragmented records, and systems that barely talk to each other. Meanwhile, AI is already at work inside Greek hospitals, quietly changing how clinicians diagnose, schedule, and manage patient care. This guide breaks down the specific tools being used right now, the real efficiency gains being recorded, and the honest challenges still standing in the way. Whether you are a clinician looking to sharpen your diagnostic workflow or a manager trying to cut operational waste, what follows is a practical look at where AI stands in Greek healthcare today.
Table of Contents
- How AI is transforming healthcare delivery in Greece
- AI-powered decision support and rare disease detection
- Operational efficiencies: Scheduling, resource management, and automation
- Challenges and ethical considerations in implementing healthcare AI
- Why successful AI adoption starts with people, not just technology
- Explore more healthcare innovation with Medical Management
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| AI tools are already in use | AI assistants and data platforms are supporting clinical and administrative work in Greek hospitals. |
| Efficiency gains are substantial | AI technology accelerates clinical processes, cuts costs, and improves patient outcomes when well-integrated. |
| Challenges require attention | Data fragmentation, staff training, and ethical concerns are significant barriers to broader AI adoption. |
| People make the difference | The success of AI depends on clinician engagement and organizational culture—not just advanced software. |
How AI is transforming healthcare delivery in Greece
Greek healthcare has long struggled with administrative overload and disconnected digital infrastructure. AI is beginning to address both problems at once, and the results are measurable.
One of the most significant developments is the Digital Doctor Assistant in Greek NHS, which enables natural language queries directly within the national electronic health record system. Instead of navigating complex menus, doctors can simply ask the system a question in plain Greek and receive relevant patient data instantly. This alone saves meaningful time during busy outpatient shifts.
At the same time, platforms like myHealthDoc are expanding access to national EHR data for clinicians working across different settings. For a country where continuity of care has historically been fragmented, this kind of integration matters enormously. You can read more about how a new health services platform is reshaping access to care in Greece.
Beyond record access, AI is accelerating clinical research and hospital operations. Consider these figures:
- AI accelerates clinical trials by 30 to 50%, cuts costs by 40%, and boosts patient recruitment by 65%
- AI-powered scheduling tools reduce staff idle time and improve shift coverage
- Automated coding and billing systems cut claim errors and speed up reimbursements
| AI application | Key benefit | Impact area |
|---|---|---|
| Natural language EHR queries | Faster data retrieval | Clinical workflow |
| Predictive scheduling | Optimized staff allocation | Operations |
| Automated billing | Fewer claim errors | Administration |
| Clinical trial matching | Faster patient recruitment | Research |
These are not future projections. Greek hospitals are already piloting these tools, and the early data is encouraging. The ChatGPT support for healthcare model is also being explored for personalized patient guidance, adding another layer of AI utility to the clinical ecosystem.
AI-powered decision support and rare disease detection
Beyond operational improvements, AI’s true clinical power shines in supporting doctor decision-making and diagnosing complex conditions.
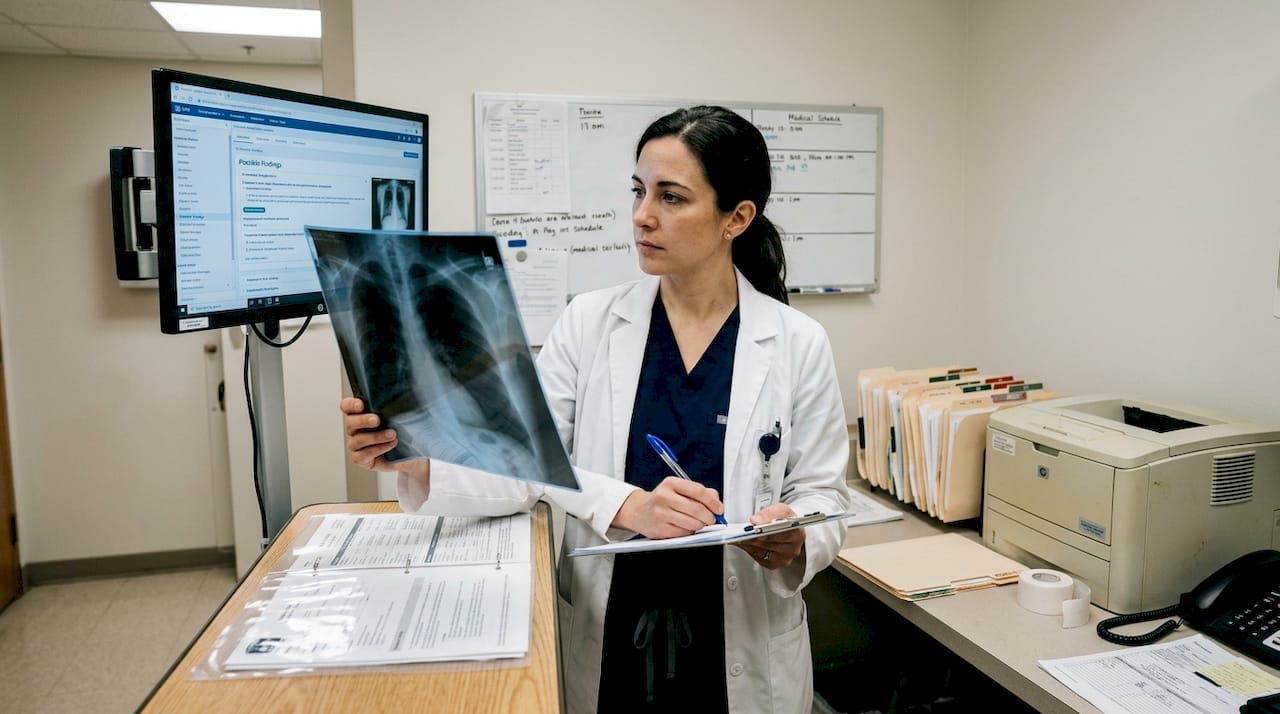
One striking example comes from a rural Greek practice. A doctor used AI to help identify Q fever, a bacterial infection that is notoriously easy to miss. The AI flagged subtle symptom combinations and environmental exposure data that might not have triggered immediate suspicion through a standard differential diagnosis process. As AI for diagnosis in Greece shows, without AI, Q fever might not have made the shortlist at all.
Here is how a typical AI-assisted diagnostic workflow looks in practice:
- Patient history input: The clinician enters symptoms, exposure history, and relevant labs into the system
- Pattern recognition: The AI cross-references thousands of similar cases and flags possible diagnoses ranked by probability
- Drug interaction check: The system automatically screens for contraindications based on the patient’s current medications
- Guideline alignment: The AI suggests relevant clinical guidelines for the top diagnoses
- Final decision: The doctor reviews the AI output and applies clinical judgment to confirm or adjust
Comparing traditional and AI-supported workflows makes the difference clear:
| Workflow step | Traditional approach | AI-supported approach |
|---|---|---|
| Rare disease flagging | Relies on doctor recall | Automated pattern matching |
| Drug interaction check | Manual reference lookup | Instant automated screening |
| Guideline retrieval | Time-consuming search | Integrated, real-time suggestions |
| Documentation | Manual entry | Partially automated |
The critical point here is that AI is an assistant, not a replacement. As explored in the discussion around AI and human judgment, the technology supports clinicians rather than substituting for their expertise.
“AI gives me a second opinion at 2 a.m. when there is no colleague to call. It does not decide for me, but it makes sure I have not missed something obvious.”
Pro Tip: Use AI decision support tools as a structured checklist during complex cases, not as a final authority. Treat the output the same way you would treat a knowledgeable colleague’s suggestion: worth considering, not automatically correct.
Operational efficiencies: Scheduling, resource management, and automation
While decision support is vital, AI is also quietly transforming the backbone of healthcare operations.
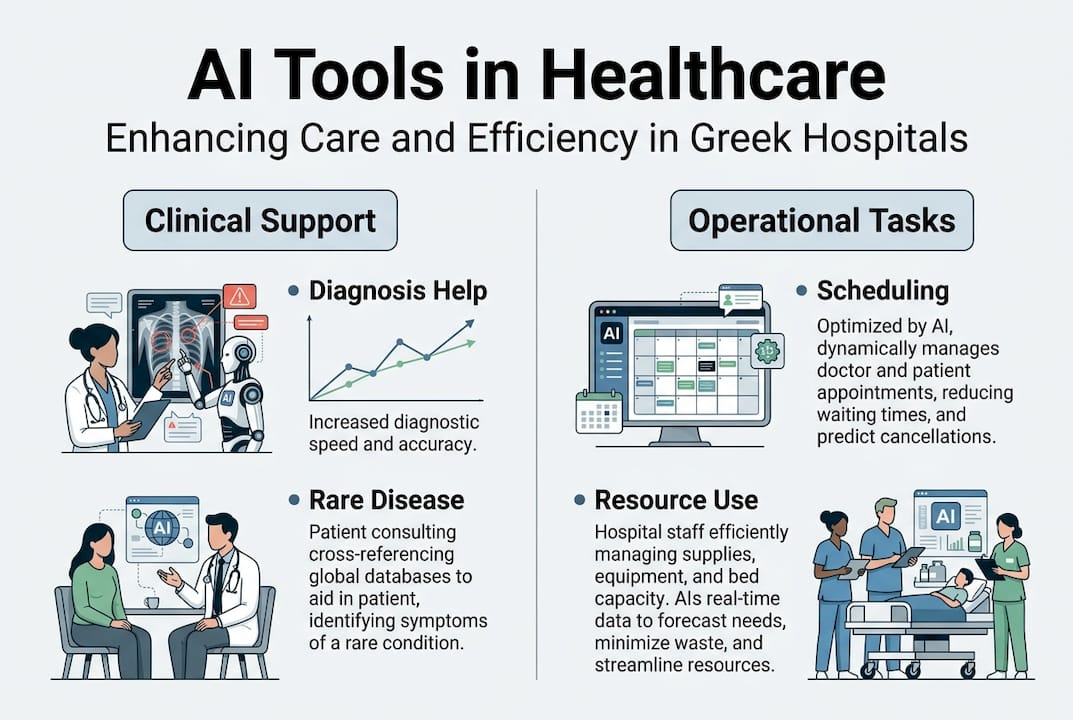
Greek hospital managers are under constant pressure to do more with less. Staff shortages, budget constraints, and unpredictable patient volumes make traditional scheduling methods unreliable. AI-driven tools are changing this by analyzing historical patient flow data to predict busy periods and automatically adjust staffing levels before a crisis hits.
Key operational areas where AI is making a measurable difference include:
- Workload balancing: AI distributes patient assignments more evenly across nursing and support staff, reducing burnout
- Predictive resource allocation: Supplies and equipment are ordered based on forecasted demand, cutting waste
- Automated administrative tasks: Appointment reminders, discharge summaries, and routine correspondence are handled automatically
- Trial design acceleration: AI-driven operational efficiency produces 30 to 50% faster trial design and up to 40% lower costs
Despite these gains, the infrastructure challenge is real. Only 14% of Greek hospitals have fully integrated EHR systems, and dissatisfaction with current digital tools remains high among staff. The push toward digitized hospital systems is a necessary foundation before AI can reach its full operational potential.
Pro Tip: Before investing in AI scheduling tools, audit your current data collection practices. AI is only as reliable as the data it learns from. Inconsistent or incomplete records will produce unreliable recommendations.
The hospitals seeing the strongest results are those that treated AI implementation as a process redesign project, not just a software installation. That mindset shift matters more than the specific tool chosen.
Challenges and ethical considerations in implementing healthcare AI
With so much promise, it is important to address the real-world challenges and ethical questions that come with AI adoption.
The biggest structural barrier in Greece is data fragmentation. Only 14% have integrated EHR, and 98% of staff report dissatisfaction with current EHR connectivity. When patient data lives in silos across different hospital systems, AI tools cannot access the complete picture they need to function accurately.
Other significant challenges include:
- Bias in training data: If AI models are trained on datasets that underrepresent certain patient populations, their recommendations may be less accurate for those groups
- Regulatory gaps: Greece, like much of Europe, is still developing clear frameworks for AI accountability in clinical settings
- Staff AI literacy: While awareness is growing, many clinicians and managers still lack the practical skills to evaluate AI outputs critically
- Trust deficits: Some healthcare professionals remain skeptical about relying on algorithmic recommendations for high-stakes decisions
“The question is not whether AI is capable. The question is whether our systems and our people are ready to use it responsibly.”
Addressing these barriers requires a structured approach. Gradual integration, starting with lower-risk applications like scheduling and documentation before moving to diagnostic support, reduces the chance of costly errors. Investing in staff education is equally important. Tools like ChatGPT support for healthcare can actually serve as low-stakes training environments where staff build familiarity with AI-generated outputs before applying similar tools in clinical contexts.
Robust digital infrastructure is the non-negotiable foundation. Without it, even the most sophisticated AI tool will underperform.
Why successful AI adoption starts with people, not just technology
Here is the uncomfortable truth that most AI vendor pitches skip over: technology does not transform healthcare. People do.
Greece has seen this play out repeatedly. Hospitals that invested in digital tools without investing equally in staff readiness ended up with expensive systems that nobody trusted or used consistently. The 98% dissatisfaction rate with EHR connectivity is not just a technical failure. It is a cultural and change management failure.
Real AI success in Greek hospitals depends on involving doctors and nurses from the very beginning of any implementation project. Not as end users who receive training after the fact, but as co-designers who shape how the tool fits into their actual workflow. When clinicians feel ownership over a system, adoption rates climb and resistance drops.
User-friendly interfaces matter more than feature lists. A tool that a busy cardiologist will actually use during a 12-hour shift is worth more than a theoretically superior system that feels clunky under pressure. The progress toward digitized hospital systems in Greece is encouraging, but the pace of cultural adaptation needs to match the pace of technical rollout.
True transformation is not about having the best algorithm. It is about building a clinical environment where professionals trust the tools, understand their limits, and use them to deliver better care. That is a human achievement, enabled by technology.
Explore more healthcare innovation with Medical Management
If the examples and insights in this article sparked ideas for your own practice or hospital, there is much more to explore. MedicalManage.gr is built specifically for Greek healthcare professionals who want to stay ahead of clinical and operational developments.
From in-depth coverage of AI innovations in medicine to practical strategies to attract patients for clinic managers, the platform covers the full spectrum of modern healthcare practice. Whether you are a specialist looking for the latest diagnostic research or an administrator seeking operational frameworks, MedicalManage.gr offers the resources to help you act on what you learn. Explore the latest articles and make informed decisions that benefit both your team and your patients.
Frequently asked questions
How does AI improve diagnostic accuracy in Greek hospitals?
AI tools help Greek doctors detect rare diseases, support differential diagnoses, and flag drug interactions by analyzing complex symptom data. As demonstrated by AI for diagnosis in Greece, conditions like Q fever that might be missed in a standard review are surfaced through pattern recognition.
What are the main challenges to using AI in Greek hospitals?
The core barriers are fragmented electronic health records, low interoperability between systems, moderate staff AI literacy, and the absence of unified national regulations. Fragmented data and low EHR integration remain the most urgent structural problems to solve.
Does AI replace the role of doctors in Greece?
No. AI assists clinicians by streamlining processes and supporting clinical decisions, but it does not replace human expertise or judgment. The AI supports doctors model is consistently reinforced by both research and real-world practice in Greece.
How can Greek healthcare professionals prepare for greater AI integration?
Investing in digital literacy, participating in structured training programs, and engaging actively with hospital transformation initiatives are the most effective steps. Ongoing training and digital readiness are consistently identified as the key factors separating successful AI adopters from those who struggle.





